Release Date: 2026-04-10
Paul Li
CTO | Author18 years experience in the Research and Development of 3D printing equipment and additive manufacturing processes, empowering the efficient intelligent manufacturing of complex parts.
Introduction: The Dawn of Digital Dentistry
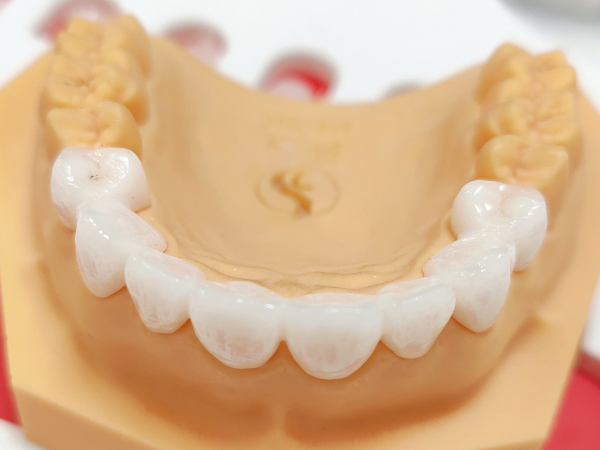
The field of dentistry is undergoing a remarkable transformation, with ceramic 3D printing at the forefront of this revolution. Once limited to traditional manufacturing methods, dental restoration has now embraced additive manufacturing technologies that offer unprecedented precision, customization, and efficiency. Ceramic 3D printing has emerged as a game-changer, enabling the creation of dental crowns, bridges, implants, and other restorations with superior mechanical properties, biocompatibility, and aesthetic appeal that are transforming how we approach dental care.
I. The Digital Transformation: From Traditional Methods to 3D Printing
For decades, dental restorations were primarily manufactured using subtractive methods such as milling or traditional casting techniques. These approaches presented several significant limitations that patients and dentists had to accept as unavoidable. Material waste was a major concern, with up to 60-70% of expensive ceramic material being discarded during milling processes. Design constraints meant that complex geometries and internal structures were difficult or impossible to achieve, limiting the potential for optimal restoration design. The time-consuming processes required multiple appointments for impression taking, laboratory fabrication, and final placement, often stretching treatment over several weeks. Perhaps most frustrating was the limited customization, as standardized approaches often failed to address individual patient needs, resulting in compromises in fit and function.
Ceramic 3D printing has fundamentally changed this paradigm by enabling a completely new approach to dental restoration. Through additive manufacturing, material is deposited layer by layer, dramatically minimizing waste and making the process more environmentally friendly and cost-effective. Complex geometries that were once impossible are now achievable, allowing for intricate internal structures and truly patient-specific designs that optimize both function and aesthetics. Rapid prototyping capabilities mean that same-day restorations are now achievable in many cases, eliminating the need for temporary crowns and multiple visits. Most importantly, personalized medicine has become a reality, with each restoration tailored to individual anatomical requirements, ensuring the perfect fit and optimal performance for every patient.
II. Key 3D Printing Technologies for Dental Ceramics
Digital Light Processing (DLP) technology has become one of the most popular methods for dental ceramic printing, revolutionizing how dental laboratories and clinics produce restorations. Using a digital light projector, this technique cures liquid ceramic resin layer by layer with remarkable speed and precision that was unimaginable just a decade ago. The resolution typically ranges from 25-50 microns, allowing for incredibly detailed reproductions of tooth anatomy. Printing speed is impressive, with a single crown taking only 15-30 minutes to complete. The materials used are sophisticated photopolymerizable ceramic slurries containing zirconia or lithium disilicate particles suspended in a resin matrix. These advanced formulations enable the production of crowns, bridges, veneers, and temporary restorations with exceptional quality and consistency.
Stereolithography (SLA) technology offers an alternative approach that employs a focused laser beam to selectively cure ceramic resin, providing exceptional precision for the most complex dental structures. The ultra-high precision of SLA systems, capable of 20-30 micron resolution, makes them ideal for applications where every detail matters. The smooth surface finish achieved through laser curing significantly reduces the need for post-processing, saving time and preserving delicate features. Complex geometries that would challenge other printing methods are handled with ease, making SLA particularly suitable for intricate implant-supported restorations. The material versatility of SLA systems allows compatibility with various ceramic formulations, giving dental professionals flexibility in material selection based on specific clinical requirements.
Material extrusion-based 3D printing represents an emerging technology that involves extruding ceramic pastes through fine nozzles, building structures layer by layer in a manner similar to traditional pottery but with digital precision. Recent developments in this field have been particularly exciting, with research demonstrating successful extrusion-based printing of fully dense zirconia ceramics for dental restorations. The multi-material capabilities of extrusion systems hold tremendous potential for creating gradient structures that combine different ceramic compositions within a single restoration, optimizing properties throughout the structure. Perhaps most appealing is the cost-effectiveness of extrusion-based systems, which typically have lower equipment costs compared to photopolymerization methods, making advanced ceramic 3D printing more accessible to smaller dental practices.
III. Advanced Ceramic Materials for Dental Applications
Zirconia (ZrO₂) has emerged as the workhorse of dental ceramics, dominating the field of 3D printed dental restorations due to its exceptional combination of properties. The mechanical strength of zirconia, ranging from 900-1200 MPa in flexural strength, makes it one of the strongest materials available for dental applications. Its biocompatibility is excellent, providing outstanding tissue compatibility with no risk of allergic reactions, which is crucial for long-term oral health. Chemical stability ensures that zirconia restorations resist degradation in the challenging oral environment, maintaining their integrity over many years. Perhaps most impressive has been the aesthetic potential of modern zirconia formulations, which now offer significantly improved translucency compared to earlier versions, allowing for more natural-looking restorations even in visible areas.
The clinical applications of zirconia are extensive and varied. Posterior crowns benefit greatly from zirconia’s exceptional strength, making it ideal for molars that must withstand substantial chewing forces. Implant-supported restorations excel with zirconia, which provides excellent performance for implant abutments and frameworks. Multi-unit bridges find zirconia particularly suitable, capable of supporting three-unit and longer-span bridges with confidence. Full-arch restorations in All-on-X implant solutions frequently utilize zirconia frameworks, taking advantage of the material’s strength-to-weight ratio and biocompatibility.
Lithium disilicate glass-ceramic represents the gold standard for anterior aesthetic restorations, where appearance is paramount. The aesthetic excellence of lithium disilicate stems from its natural tooth-like translucency and exceptional color matching capabilities, allowing restorations to blend seamlessly with surrounding natural teeth. While its moderate strength of 360-400 MPa flexural strength may be lower than zirconia, it remains more than adequate for most applications while offering superior optical properties. The excellent polishability of lithium disilicate ensures that restorations maintain a smooth surface over time, reducing plaque accumulation and enhancing long-term aesthetics. Minimal tooth preparation requirements make lithium disilicate an attractive choice for conservative dentistry approaches.
The primary uses of lithium disilicate glass-ceramic showcase its versatility in aesthetic dentistry. Anterior crowns benefit from its optical properties, making it perfect for visible front teeth where appearance cannot be compromised. Veneers crafted from lithium disilicate provide thin shells for cosmetic enhancement with minimal tooth reduction. Inlays and onlays offer conservative restorations for posterior teeth, preserving healthy tooth structure while providing durable function. Partial crowns provide targeted coverage of specific tooth surfaces, offering a middle ground between full crowns and more conservative restorations.
Advanced composite ceramics represent the cutting edge of dental material science, with recent research focused on developing formulations that combine the best properties of different materials. Innovative formulations such as Al₂O₃ whisker/3Y-TZP composites offer enhanced mechanical properties with improved low-temperature aging resistance, addressing one of the historical concerns with zirconia materials. ZrO₂/Al₂O₃ bioceramics have been optimized specifically for all-ceramic dental implants, providing the strength and biocompatibility required for these demanding applications. Gradient materials represent perhaps the most exciting development, creating structures with varying composition throughout to achieve optimal performance in different regions of a single restoration.
IV. The Complete Workflow: From Digital Design to Final Restoration
The process begins with digital impression and scanning, eliminating the need for traditional impression materials that many patients find uncomfortable. Modern intraoral scanners capture 3D tooth morphology with impressive 20-50 micron accuracy, providing detailed digital models that form the foundation for all subsequent work. CBCT integration allows these surface data to be combined with internal bone structure information, giving clinicians a comprehensive view of the treatment area. Real-time visualization capabilities enable immediate quality assessment of scan data, allowing technicians to identify and address any issues before proceeding to the design phase.
Computer-aided design (CAD) software has evolved into sophisticated platforms that enable precise restoration design with unprecedented ease and accuracy. Automated crown design features powered by AI-assisted algorithms can suggest optimal shapes based on vast databases of successful restorations, while still allowing for clinician customization. Bite analysis capabilities provide virtual simulation of occlusal contacts, allowing designers to optimize function before any material is printed. Margin detection algorithms automatically identify preparation margins with high accuracy, ensuring proper fit and seal. Aesthetic customization tools enable detailed color and translucency mapping, allowing restorations to be tailored to match surrounding teeth perfectly.
The 3D printing process itself involves several critical steps that must be carefully controlled to ensure optimal results. Layer thickness typically ranges from 25-100 microns depending on the specific application and desired resolution, with thinner layers providing greater detail but requiring longer print times. Support structures are automatically generated as temporary supports for overhanging features, preventing deformation during printing. Build orientation is strategically optimized to minimize support requirements while maximizing structural integrity. Environmental control systems maintain precise temperature and humidity regulation throughout the printing process, ensuring consistent material properties and print quality.
Post-processing and sintering represent the final transformation of printed ceramic restorations into their final, functional form. Debinding is the first critical step, involving the careful removal of organic binders from the green parts without damaging the delicate ceramic structure. Support removal follows, with temporary support structures being carefully eliminated using specialized tools and techniques. Sintering represents the most dramatic transformation, with high-temperature treatment typically ranging from 1400-1600°C causing the ceramic particles to fuse together and achieve their final density and strength. Shrinkage compensation is essential, as design adjustments must account for the 20-25% dimensional reduction that occurs during sintering. Finally, surface finishing through glazing and polishing ensures optimal aesthetics and smooth surfaces that promote oral health.
This comprehensive workflow, from initial digital scanning through final placement, represents a paradigm shift in dental restoration. What once required multiple appointments, weeks of laboratory work, and significant material waste can now be accomplished with digital precision, minimal waste, and often in a single day. The integration of advanced materials, sophisticated printing technologies, and intelligent software has created a new standard of care that benefits both patients and dental professionals alike.
About Forgecise
Forgecise is an innovator in additive manufacturing technology, dedicated to providing high-performance metal 3D printing materials, equipment, and process solutions for the mold manufacturing, energy power, and other industrial sectors.